Page Contents
Facial numbness and tingling at the back of the head and face can be referred to as having less or no sensation in the skin of these areas. This can actually happen to any parts of the body. The sensation may be felt or characterized as prickling pins and needles, creeping, and ant crawling [1]. Head numbness or face numbness is medically termed as head paresthesia [2].

Picture 1: Numbness and tingling of the head and face
Source: www.buzzle.com
What are Head Dermatomes?
A dermatome is an area of the skin which is localized. It is responsible for sensory through the nerves that arise from a single spinal nerve root.
The head dermatomes are responsible for the sensation of the face and top part of the head. The left and right trigeminal nerve links these two locations. The trigeminal nerve starts from where the brainstem is located. Also, it separates into three branches [3]. These are:
1. Ophthalmic Nerve
This runs through the top of the orbit and its entrance to the face is via the area above the eye. The ophthalmic nerve is responsible for the sensation of the areas which include: forehead, eyebrows, half of the frontal top of the head, upper eyelids, skin areas covering the top of the cornea, conjunctiva, nose, and frontal sinuses, as a result it is no surprise that a problem with this nerve can cause a numb face.
2. Maxillary Nerve
The entrance of this nerve is located below the eye. Then, it extends through the bottom part of the orbit. Also, it is responsible for sensation of the skin on the lower eyelid, nasal mucosa, paranasal sinuses, sides of the nose, cheeks, upper teeth and gums.
3. Mandibular Nerve
This branch of the dermatomes includes the inner portion of the jawbone, then, it enters the sides of chin. This also innervates the covering skin of the jaw. The mandibular nerve branch named as auriculotemporal branch stimulates the front of the earlap, as well as the temporal portion.
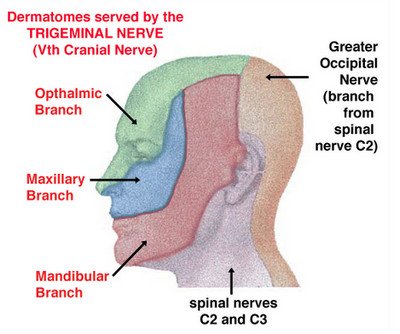
Picture 2: Head Dermatomes
Source: users.bergen.org
On the other hand, the dermatomes responsible for the back of the head sensation involve cervical nerves C1-C3. As for neck and majority of the earlap, their sensitivity is supplied by the cervical nerves C1-C4 that makes up the superficial cervical plexus. [4]
What are the causes of numbness and tingling at the back of head and face?
The paresthesia of the head and face are mainly caused by irritation of the nerves such as: cervical (C1-C4) nerves, nerves at the brainstem, trigeminal nerve, and spinal cord. Other parts of the brain which are responsible for the head/face sensitivity may also be affected when the nerves become irritated.
1. Neurological Disorders
When the nervous tissues are affected by the neurological disorders, it usually leads to the occurrence of numbness and tingling. This is most commonly located at the back of the head and face. These disorders include:
- Herpes Zoster (Shingles): This disorder involves reoccurring of chicken pox virus. This happens when they particularly attack the nerve roots of the trigeminal or cervical nerves. The reoccurrence of this disease manifests as a tingling sensation felt at certain parts of the body such as scalp, one side of the face, and body trunk.

Picture 3: Common sites where shingles occur
Source: specialityclinic.com
- Post-herpetic Neuralgia: This condition results from the complication of the reoccurrence of Herpes Zoster. The reactivation of Herpes Zoster usually happens to patients who are over 50 years of age. The facial numbness, tingling, or pain may remain for several months or even years.
- Trigeminal Neuralgia (tic douloureux): This is a chronic disorder of the nerves that mostly affects adults. The origin is unknown but it may cause problems such as sudden severe shock-like (or mild) facial pain. This may be triggered by factors which involve touching or movement of the face such as shaving, chewing, laughing, speaking, tooth brushing, and slight breeze. The tingling and numbness occur before this type of pain occurs.
- Anesthesia Dolorosa: This involves facial numbness and constant stabbing pain that occurs as a treatment complication of trigeminal neuralgia.

Picture 4: Pain experienced in Trigeminal Neuralgia
Source: uthealthleader.org
- Trigeminal Neuropathic Pain: This can be a result of trauma, surgery, dental procedure, or disease such as stroke or diabetes. It manifests with symptoms which include long-lasting dull pain which can be described as burning. The condition may also cause manifestation of symptoms such as numbness or tingling.
- Trigeminal Deafferentation: This is referred to as the interruption of the sensory nerve fibers. This results from damage of the nerves. The nerve damage usually occurs during the course of treatment for trigeminal neuralgia such as alcohol injections and surgery. It is characterized by burning numbness which is continuous.
- Lyme Disease: It is caused by an infection from a tick bite. After months or years of the tick bite, manifestations of tingling and paralysis of the facial muscles may occur.
- Multiple Sclerosis (MS): This is an autoimmune disorder which involves the brain and the spinal cord. This commonly occurs in patients who are 20-40 years of age. It commonly manifests as a one-side paralysis of muscle weakness of the body.
- Guillain-Barre Syndrome: This is a rare disorder that affects the immune system. It may develop after days or weeks of having a respiratory infection or food poisoning. This disease targets the peripheral nerves. The muscular weakness and numbness progresses in an ascending manner. It starts from the feet towards the trunk and going to head.
- Epilepsy: When neurons or brain cells have an abnormal electrical activity, this causes irritation of the nerves. As a result, this leads to episodes of convulsions, muscle spasms, and even loss of consciousness. Before the convulsions occur, tingling, numbness, change of taste or smell, and strange emotions or behaviour may be experienced by the patient.
- Syphillitic myelopathy (Tabes Dorsalis): This condition results from a rare complication of untreated syphyllis. It involves abnormal sensations described as lightning pains, muscle weakness, and loss of reflexes.
2. Psychological Disorders
- Anxiety and Panic Attack: A person who is having anxiety and panic attack has an experience of extreme fear. Also, tingling or numbness certain parts of the body commonly in the hands, feet, legs, face, arms, and other body parts may be felt.
3. Allergies/Poisoning
- Food Allergies: This causes tingling felt on the lips. It also results to swelling of the face and itching of the throat and skin.
- Seafood poisoning: Leads to tingling, skin rash, and diarrhea.
4. Cerebrovascular/Circulatory Disorders
- Stroke/ Transient Ischemic Attack: These conditions occur when there is an occlusion or rupture of a brain artery due to atherosclerosis, thrombosis, or aneurysm. It manifests as having numbness or weakness of the arm, leg, and arm.
- Vertebrobasilar Circulatory Disorders: This happens due to blood supply occlusion to the brain.
- Angina Pectoris: It is described as a pain located at the back of the breast bone which may be sharp or dull. This sensation may radiate or crawl to the hand, arm, left shoulder, or jaw.
- Vasculitis: When the small to medium sized arteries are inflamed, head tingling and numbness may result.
5. Spinal Disorders:
Spinal Disorders that are known to have an effect to the cervical nerves which are above C4 level are known to cause head paresthesia. Examples of these disorders are:
- Osteoporosis
- Spondylitis or vertebral inflammation
- Herniation of the spinal disc
- Degenerative Disc Disease
6. Injuries
- Spinal Cord Injuries: Specifically affecting the cervical spine above the C4 level
- Injury of the head or facial bones: Cuts, punctures, bruises, fracture
- Dislocation of the jaw
7. Tumors
- Growth of tumors at the brain, ear, nose, orbit, paranasal sinuses, mouth, parotid glands, skull, vertebra, spinal cord, muscle or skin
8. Metabolic Disorders
- Electrolyte imbalances such as low levels of calcium
- Hypoglycemia (low sugar levels in the blood)
- Uremia (bacteria in urine)
9. Medications/Drugs/Toxins
- Anticonvulsant drugs, HIV medications
- Chemotherapy drugs, Radiation therapy
- Alcohol
- Tobacco
- Poisoning: Snake bites, seafood poisoning, heavy metal poisoning (lead, mercury, arsenic), nitrous oxide [4]
Diagnosis of Numbness and Tingling at Back of Head and Face
The diagnostic test that could be used for the evaluation of numbness or tingling at the back of head and face depends on the determined underlying condition [5].
1. Medical Interview
The doctor will be asking some questions to determine about the history of the patient’s symptoms. The interview will include:
- Location: This will include where the numbness or tingling is occurring. It may be affecting one or both sided areas or if it is symmetrical or non-symmetrical.
- Time Course: The doctor will ask when did the symptoms started manifesting, how long it lasts, if it is recent or long lasting, constant, or changes over time.
- Other symptoms: This portion would include symptoms affecting senses, temperature, balance, eating, speech, and movement. Also, the doctor will ask if the patient has been experiencing pain, nausea, fever, cramping, or paralysis.
- Health History: The doctor will check the patient’s history. If he/she has a history of diabetes, , cancer, vascular disease, alcohol abuse, or trauma.
- Family History: The patient will also be asked if there have been a history of paresthesia occurring in the family. [4]
2. Physical Examination
- Neurological Examination: This will be performed by a neurologist. [4]
3. Laboratory Tests
- Blood tests: Complete Blood Count, Electrolytes, Thyroid Stimulating Hormone (TSH), Blood Urea Nitrogen (BUN), haemoglobin, vitamin B12, thiamine, ESR
- Urine tests
- Nerve biopsy
- Nerve conduction studies [4, 6]
4. Imaging Studies
- Chest X-ray
- CT Scan/MRI/Nuclear Scans
- Electromyography (EMG): This is ordered by the doctor to differentiate neuropathic versus myopathic causes of muscle atrophy [4, 6]
Treatment of Numbness and Tingling at the Back of Head and Face
1. Treating the Underlying Cause
- The treatment of this condition aims diagnosing and treating the determined underlying cause. There are some conditions which could be easily treated and cured. On the other hand, there are also conditions which may require intensive treatment and may not have a good prognosis.
- If the underlying cause is due to a chronic disease or treatment complications like in chemotherapy, the treatment will be focused on the relief of the patient’s symptoms.
- For patients with more severe cases of facial numbness and tingling of the head, they are given antidepressant medication such as amitriptyline. This is given in a lower dosage to help the patient with his/her perception of pain.
- Anti-inflammatory drugs: This includes NSAIDS or steroids.
- Analgesics
- Nutrition therapy (B complex vitamin supplementation)
- Avoiding alcohol consumption and drug abuse
- Helping the patient cope effectively [4, 5, 6]
2. Stress Relief
3. Alternative Treatment
- Other treatment may include exercising, stretching, or massaging the affected area. This helps in promoting circulation in the body.

Picture 5: Relieving stress as one of the ways to prevent paresthesia
Source: healthtap.com
- Acupuncture and Massage: These are believed to cure symptoms.
- Self-massage with aromatic oils: In doing this, using topical ointments such as the ones containing capsaicin, provides relief from paresthesia.
- Wear loose-fitting clothes and shoes. [5]
References:
1. http://www.healblog.net/numbness-and-tingling-in-the-back-of-the-head-and-face
2. http://www.livestrong.com/article/151353-causes-of-head-numbness/
3. http://emedicine.medscape.com/article/1878388-overview
4. http://www.healthhype.com/tingling-and-numbness-in-the-face-and-back-of-the-head.html
5. http://www.disabled-world.com/health/neurology/paresthesia.php
6. http://www.rightdiagnosis.com/p/paresthesia/





I am writing onbehalf of my father who is 54 years old and is facing numbness on half the right side of the face only and the doctors are saying MRI result is nill.and this happened while he got a sudden shock (not electrocuted but he got scared) and felt dizzy while he was standing under electric powerlines and the two wires got conected by a digger and it sparked and blew off with a heavy sound,that’s the time he felt dizzy and the next day he got that weakness.is there any solutions to it or how could it be cured??
I have tingling on my whole body it’s worse on my face because my cheeks burn and the inside of my mouth burns as well. It is driving me crazy and what makes it even worse is I have no clue what it is. Sometimes it’s so bad it’s hard to swallow and I get choked. My doc says I have allergies.
My pins and needle feeling start at the top of my head and work their way down my body with a residual amount in my face.
Last night the pins and needle feeling stayed in my face longer than usual and my entire faced swelled up.I looked like someone in a horror movie.when I get these attacks , I am never worried or anxious about anything.
This is the same thing happening to me except it’s mainly the right side, I also get a burning sensation, and the right side of my face goes numb.
I have numbness in my head, face, shoulders and radiating to the upper torso, to elbows. I have dizzy spells this all started after I popped my neck. when I wake in the morning its not so intense until I get to work and start lifting or reaching over my head. I’m still waiting on an MRI – my PCP sent me for xray where I have a bone spur attached to where I had a fusion. Is this the connection to the numbness? but If I take a muscle relaxer I’m in so much pain I cannot stand myself so I guess I would rather be numb!? But there is a problem and I would just like to know what it is