Page Contents
Hyponatremia Definition
Hyponatremia is an imbalance in electrolytes, where there is low serum sodium than the normal level.
- Normal – 136-145 mEq/L
- Hyponatremia – <135 mEq/L
- Severe hyponatremia – <125 mEq/L
It is one of the common and essential electrolyte abnormalities, which can either be present in isolation or as a resultant complication of the several medical conditions. Excess water in the body dilutes the sodium in blood by getting accumulated within the body, including congestive heart failure, polydipsia or SIADH (syndrome of inappropriate antidiuretic hormone), and sometimes it can also be seen in over-hydration.
Inadequacy of sodium intake is rarely the cause for hyponatremia; but this may an indirect cause. The antidiuretic hormone that gets released, stimulates the water retention, making the sodium into the blood diluted, thereby resulting in hyponatremia. When the sodium gets diluted, the cells swell, and this can cause many health problems.
Hyponatremia Epidemiology
- Frequency: Females > males
- Commonly seen in hospitalized persons and the elderly, as they are more likely to suffer from the co-morbidities like a cardiac, renal or hepatic failure.
- 3-5 % of the total hospitalized individuals have < 130 mEq/L
- 30 % of the total depressed people, who are on serotonin re-uptake inhibitors suffer from hyponatremia.
Hyponatremia Pathophysiology
Pathophysiologically, hyponatremic etiology is categorized in 3 ways, according to the plasma osmolality of a patient.
1. Hypertonic hyponatremia:
It is caused due to the water resorption that is drawn by the so-called osmols like mannitol, i.e., hypertonic infusion, or glucose (diabetes or hyperglycemia).
2. Isotonic hyponatremia:
This is nothing, but the pseudohyponatremia that occurs due to lab error, commonly as a result of hypertriglyceridemia and hyperparaproteinemia as well.
3. Hypotonic hyponatremia:
This being the most common, is used conversely with the condition hyponatremia, and according to the blood volume of the patient, hypertonic hyponatremia is classified into 3 types, where each category symbolizes another cause for the increased ADH leading to retention of water, thereby causing hyponatremia. Hence, it is classified as,
a. Hypervolemic hyponatremia:
Here, even though, there is an increased volume within the body due to edema, effective circulating volume is decreased. Thus, the decreased circulating volume activates ADH release that in a way leads to retention of water. Hence, this resultant hypervolemic hyponatremia is due to liver cirrhosis, nephrotic syndrome or even congestive heart failure.
b. Euvolemic hyponatremia:
The ADH increase occurs followed by physiological release of excessive ADH (seen in pain or nausea), or non-physiological inappropriate ADH secretion, i.e., SIADH.
c. Hypovolemic hyponatremia:
Here, volume depletion stimulates ADH secretion.
- However, this volemic classification does not succeed in including the artifactual hyponatremia that is included under the classification of osmolars. E.g.: Severe hyperglycemia, immunoglobulin level elevation and hypertriglyceridemia.
- In case of acute hyponatremia, there is a rapid drop in the sodium level that causes dangerous complications like brain swelling resulting in coma and even death.
- In case of chronic hyponatremia, there is a gradual drop in the sodium level for many weeks and still causing only moderate symptoms as well as complications. Hence, it is called as asymptomatic hyponatremia, believing that it doesn’t possess any symptoms. But, the truth is that this type of hyponatremia is not asymptomatic in actual.
Hyponatremia Types
In hyponatremia, the imbalance existing between water and sodium in the blood can be depicted in 3 ways:
- Euvolemic hyponatremia – Even though the total water content in the body increases, the amount of sodium does not undergo any change.
- Hypervolemic hyponatremia – The amount of water and sodium increases, but the amount of water gained is more compared to sodium.
- Hypovolemic hyponatremia – In the body, both sodium and water are lost, but the sodium may be lost via renal or non-renal routes.
- Redistribution hyponatremia – Water moves from ICF to ECF compartment, diluting the sodium. Hence, the total body sodium and water do not change in proportion. E.g.:- hyperglycemia as well as mannitol administration.
- Pseudo hyponatremia – Excess lipids or proteins dilute aqueous phase. But, the total body sodium and water do not change in proportion. E.g.:– hypertriglyceridemia as well as multiple myelomas.
Hyponatremia Causes
Depending on the types of hyponatremia, the causes, particularly of hyponatremia is as follows:
Hypervolemic hyponatremia:
- Congestive heart failure
- Cirrhosis
- Massive edema of any cause
- Nephrotic syndrome
Euvolemic hyponatremia:
- Nausea
- Severe pain
- Trauma or brain damage
- Glucocorticoid deficiency
- SIADH and its causes
- Hypothyroidism
Hypovolemic hyponatremia:
- Decreased oral consumption
- Prolonged vomiting
- Severe diarrhea
- Diuretic use (this causes a volume depletion that releases ADH)
- Miscellaneous
Malnourished state like beer potomania. Here, poor intake of protein causes inadequate formation of urine solute, which impedes the ability of the kidney to carry out the excretion of free water.
Primary polydipsia. Here, the required urine solute for excreting huge amount of water ingested exceeds beyond the ability of the body for producing it. It takes place in cases of ≥ 12 liters being ingested every day.
Factitious hyponatremia (this is due to excess increases of triglyceride in the blood, hyperglycemia, and immunoglobulin elevation in multiple myeloma).
Adrenal insufficiency and hypothyroidism (both cortisol and thyroid hormone are required for the excretion of free water).
Hyponatremia Symptoms
- Headache
- Restlessness
- Fatigue
- Vomiting
- Loss of appetite
- Nausea
- Muscle weakness
- Convulsions
- Muscle cramps or spasms
- Irritability Abnormal mental status
- Decreased consciousness
- Hallucinations
- Confusion
- Possible coma
Hyponatremia Diagnosis
Diagnostic strategy
- Evident hyponatremia.
- Inadequate elevation of urine osmolality (more than 100 microosmol per kg), usually greater plasma osmolarity.
- Plasma hypo-osmolality becomes proportional to the hyponatremic states
- Euvolemia
- Existing urine sodium ions greater than 40 millimolar per liter, but with salt intake in the normal state.
- Normal adrenal as well as thyroid function.
A physical examination needs to be performed to determine the symptom’s cause, followed by certain Blood tests and urine tests for confirming hyponatremia.
- Osmolality blood test
- Comprehensive metabolic panel (this includes serum sodium as well)
- Urine sodium
- Urine osmolality
Laboratory Studies
Urine osmolality
This helps in differentiating between conditions correlating to impairment in excretion of free water and also primary polydipsia, where excretion of water must be normal along with an intact kidney functioning. It is in malnutrition that primary polydipsia occurs and osmolality gets diluted maximally, usually < 100 microosmoles/kg. If the urine osmolality > 100 microosmole/kg, then it’s indicative of kidney’s impaired functioning in diluting the urine. This is caused after ADH levels get elevated.
Serum osmolality
This test is useful in differentiating among pseudohyponatremia and true hyponatremia, as a result of hyperlipidemia, hypertonic hyponatremia or hyperproteinemia related to glucose elevation, glycine (post-gynecologic or posturologic), mannitol, maltose(included in formulations of IgG), sucrose, etc.
Urinary sodium
This test assists in distinguishing between hyponatremia occurring as a result of hypovolemia as well as SIADH. If associated with the salt-wasting syndrome SIADH, the amount of sodium in urine measures
Plasma osmolality
275 – 290 microosmol/kg: normal
If greater than 290 microosmol/kilogram, E.g.:- Hyperglycemia or administration of mannitol
If 275 – 290 microosmol/kilogram: E.g.:- Hyperproteinemia or hyperlipidemia
If less than 275 microosmol/kilogram: E.g.:- Eval volume status
If plasma osmolality less than 275 microosmol/kilogram
Hypervolemic:– Congestive heart failure, nephrotic syndrome or cirrhosis
Euvolemic : – Hypothyroidism, postoperative states, SIADH, beer potomania,
Hypovolemic :-Skin, GI loss, diuretics, 3rd spacing
Ancillary tests
- Serum uric acid
Uric acid in the blood can be diagnostic measures, as it is decreased in SIADH. Hence, once hyponatremia is corrected, hypouricemia also gets corrected but with an existing salt-wasting mechanism.
- Serum cortisol and TSH level:
These tests are performed if hypothyroidism or hypoadrenalism is suspected.
- Serum albumin, a serum protein electrophoresis and triglycerides:
This is dependable on the patient.
CT and chest x-ray:
To rule out the cause of hyponatremia in patients with salt wasting in the cerebrum and SIADH
ECG changes:
Non-ischemic elevation of ST wave.
Hyponatremia Algorithm
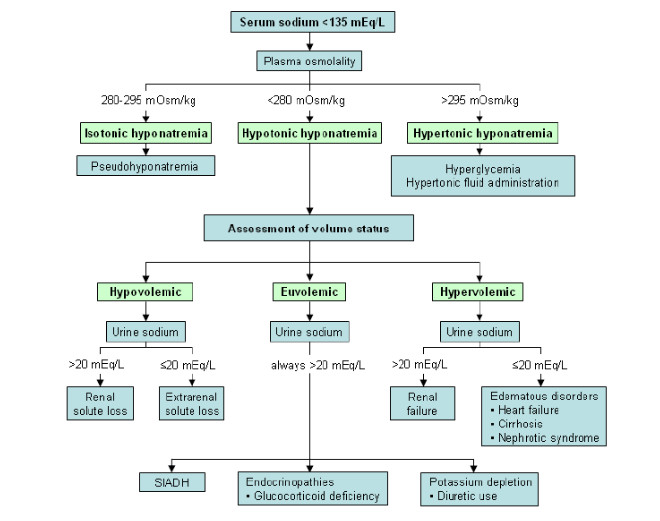
Hyponatremia Calculator
- Sodium deficiency = (desired sodium – current sodium) x 0.6 (body weight)
- Sodium ion requirement (millimoles) = (desired sodium ion – serum sodium ion) x total body water
 Insensible water loss = 500 to 1500 cc/day. Fever causes an increase in insensible water losses by 10% per degree Celsius when above 38°
Insensible water loss = 500 to 1500 cc/day. Fever causes an increase in insensible water losses by 10% per degree Celsius when above 38°
Or
- 100 to150 cc/day increment per degree Celsius when above 37°.
Hyponatremia Risk factors
Common risk factors include:-
- Age: Hyponatremia is more commonly seen in adults. The contributory factors comprise of age-specific changes and the probability to develop chronic diseases, which affects the sodium balance of the body.
- Drugs: Drugs like Thiazide diuretics, painkillers and antidepressants produces an urge in the patient to perspire or urinate more compared to normal situations.
- Conditions decreasing the excretion of water in the body: These conditions increase the hyponatremia risks, and SIADH, kidney disease and heart failure are some of the conditions.
- Vigorous physical activities: Individuals drinking excess water during ultra-marathons, marathon and triathlons or any such long-distance races increase the hyponatremia risks.
- Diet: A diet low in sodium may cause hyponatremia.
- Climate: Exposure to hot climatic conditions makes the sodium in the body to get depleted through perspiration.
Hyponatremia Differential diagnosis
- Adrenal Crisis
- Cirrhosis
- Alcoholism
- Pulmonary Edema, Cardiogenic
- Hypothyroidism
Hyponatremia Treatment
- The initial step involved in the hyponatremia treatment is the calculation of total body water
- TBW = body weight x 0.6
- The aim of the treatment is to resolve the fundamental medical condition.
- Initially correct the cause of hyponatremia by stopping the diuretics.
- In case of significant severe hyponatremia is present, consult an expert medical professional.
- Check the sodium level in the blood often for ensuring a safe correction rate of 8 to 10 millimoles/Liter per day.
- In a comatose hyponatremia patient, the acceptable rise initially to cease the severe hyponatremic symptoms would be less than 4 to 6 mmol/liter in 1 to 2 hrs.
- In moderate type of hyponatremia, the sodium correction depends on the status of the fluid.
Hypovolemic:
- Administer desmopressin, which is an ADH analogue with or without 5% glucose to suppress the ADH, so that the diuretics can elevate sodium rapidly.
Normovolaemic:
- Fluid is restricted to 500 to 1000 ml per day. If inadequacy is noted, oral NaCl tablets of 3 gm per day or 3% of IV saline is prescribed. But, if, 0.9% saline is given, then the osmolality of urine exceeds the osmolality of plasma.
Furosemide
Vaptans
Demeclocycline
Hypervolaemic:
- Fluid is restricted to 500 to 1000 ml per day with or without ACE inhibitors without furosemide.
- Given KCl raises the sodium during trans-cellular shifting of ion of Cl-, K+ and H+
Medication:
- IV fluids containing high sodium concentration and/or involving diuretics for raising the sodium in the blood.
Loop diuretics
- These water pills aim at raising the sodium levels in the blood. This is done by making the patient urinate the extra liquid from the body. IV fluids having high sodium level replaces the lost fluid or free water.
E.g.:- a. Furosemide like Lasix used either as an individual or combination drug.
b. Demeclocycline
- AVP receptor antagonist
For e.g. Conivaptan
Hyponatremia Prognosis
- Prognosis is highly dependent on the fundamental medical condition, which causes hyponatremia.
- Acute hyponatremia occurring < 48 hours is more severe and life-threatening than gradually developing hyponatremia.
- In chronic cases, the brain cells are allotted the time for adjusting, and hence, swelling is very minimal.
Hyponatremia Complications
Mild hyponatremia:
- Falls
- Gait disturbances
- Bone mass reduction
Severe hyponatremia:
- Cerebral edema
- Brain herniation
- Rhabdomyolysis
- Respiratory arrest
- Seizures
- Possible coma
- Death
Hyponatremia Prevention
- Hyponatremia can be prevented if the underlying medical condition is well-treated.
- Athletes should drink fluids containing electrolytes, especially sports drinks, as consumption of only water during sports activities that involve high-energy events result in acute hyponatremia.
References
http://en.wikipedia.org/wiki/Hyponatremia
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001431/
http://emedicine.medscape.com/article/242166-overview
http://www.mayoclinic.com/health/hyponatremia/DS00974
http://www.nlm.nih.gov/medlineplus/ency/article/000394.htm
http://www.aafp.org/afp/2004/0515/p2387.html
http://www.patient.co.uk/doctor/Hyponatremia.htm
http://circ.ahajournals.org/content/112/24_suppl/IV-121.full
http://www.medcalc.com/sodium.html




Dear
I am prof. Dr. Saad S Al Ani ,I am in process of publishing a notebook on paediatric for undergraduate and I want to copy the algorithm on hyponatremia after your permission and I will refer to you as a reference
sincerely yours
Prof. Dr. Saad S Al Ani
Ok, no problem.